Osteoarthritis of the hip joint is a complex pathology that can cause dangerous health consequences.
In order to slow down the development and treat dangerous symptoms, it is necessary to consult a doctor in time. The specialist makes the correct diagnosis and selects the appropriate treatment.
Clinical picture and classification of pathology
The pathology is progressive and involves the destruction of the bones and cartilage of the hip joint. In medicine, this disorder is often called coxarthrosis. The ICD-10 classification falls under code M16.
Most often, the pathology occurs in people over 40 years of age, and women are more susceptible to it.
In the elderly, the disease is associated with the natural aging of the body. In young people, the cause of the disease can be traumatic injuries, excess weight, increased physical activity.
In the initial stages of the disease, there are periodic pains in the joint area. Without proper therapy, the disease progresses, which can cause disability.
Causes and provoking factors
The pathology develops gradually and is associated with various factors. The following factors lead to the appearance of the disease:
- Hormonal imbalance - can be age-related or pathological.
- Violation of blood flow - occurs as a result of injuries, increased physical exertion, vascular pathologies.
- Inflammation - observed with arthritis.
- Excess weight - increased load on the hip joint provokes its compression and destruction.
- Genetic predisposition - abnormalities in the structure of the femoral head often lead to arthrosis.
- Increased physical activity - rarely provokes arthrosis, but can accelerate the development of the disease under the influence of other harmful factors.
- Traumatic injuries - this includes sprains, fractures, dislocations.
Stages and types of arthrosis

There are several stages in the development of pathology:
- The first stage - in this stage unpleasant sensations appear periodically. The provoking factor is prolonged physical activity. After a short rest, the discomfort subsides.
- The second stage - the pain in the hip joint increases, which affects the groin and thigh. Discomfort also occurs at rest. Lameness occurs after prolonged movement. In this stage, the function of the joint suffers, and its motor activity decreases. Contractures develop gradually, strength and muscle mass decrease.
- The third stage - the pain syndrome is constant and appears even at night. Walking without a cane is very difficult. The movements are disturbed and sharply limited, there is hypotrophy of the muscles of the buttocks, thighs and lower legs. When moving, a person should lean on the toes and lean on the injured side.
- The fourth stage - in this stage, the hip joint completely loses motor activity.
Symptoms and manifestations
With the development of this type of arthrosis, the following manifestations occur:
- Severe pain in the area of the affected joint and knee. In addition, there may be discomfort in the groin. The pain is constantly present. As the disease worsens, it affects the legs.
- Violation of motor activity. Excruciating pain syndrome interferes with a person's movement. In this situation, you must use a cane or crutches.
- Abbreviation of affected limb.
- Lameness.
- Crackling in the joint, which appears with any movement.
- Stiffness of movements.
- Atrophy of the muscle tissue in the thigh area - can be detected by X-ray.
Methods of diagnosing the hip joint
When making a diagnosis, the doctor takes into account the clinical manifestations of the pathology, the anamnesis, the results of the patient's external examination and instrumental tests.
In order to make an accurate diagnosis, the following tests must be performed:
- Analysis of patient complaints and external examination of the damaged area.
- X-rays can be used to identify the size of the joint gap, bone growth, etc.
- Ultrasonic procedure.
- Blood test.
- Magnetic resonance imaging.
If necessary, the inner surface of the articulation is examined with arthroscopic instruments. The differential diagnosis is performed to exclude gonarthrosis, lumbosacral or thoracic osteochondrosis. The pain occurring in arthrosis can be disguised as a clinical manifestation of radicular syndrome caused by pinching or inflammation of the nerve. Neurogenic pathology can usually be ruled out with the help of a number of tests. Arthrosis of the hip joint necessarily differs from trochanteric bursitis of the hip joint, Bechterew's disease, reactive arthritis. In order to rule out autoimmune pathologies, we perform biochemical tests of blood and synovial fluid.
Treatment
For the treatment of arthrosis of the hip joint, a combined therapy must be chosen.
General recommendations for daily routine and nutrition
In the initial stages of the pathology, the doctor advises you to change your lifestyle. This helps stop the pain and stop the progression of the disease. At this stage, it is usually sufficient to correct your lifestyle and follow a special diet.
The doctor recommends the patient to perform special physical exercises. Correcting the diet is equally important. If you are overweight, you definitely need to lose weight. Increased use of the joint does not make it possible to eliminate arthrosis.
The basis of the diet should be fish. We can also eat lean meats, legumes, green vegetables, and coarse bread. At the same time, it is recommended to avoid fried foods and fast foods. It should be eaten in portions, in small portions.
Conservative therapy

The aim of medical treatment is to solve the following problems:
- pain relief;
- normalization of tissue nutrition;
- stimulation of the regeneration process;
- improved blood flow;
- reducing pressure in damaged areas;
- enlargement of the joint space.
To solve these problems, you should use the following drug categories:
- Nonsteroidal anti-inflammatory drugs. These drugs relieve pain and inflammation. However, they cannot restore the affected cartilage.
- Chondroprotectors. They provide nutrients to the tissues and stop the destruction of the joints, which helps to restore their functions.
- Muscle relaxants. With the help of such foundations, muscle tissue spasms can be eliminated and blood flow in the tissues can be normalized.
- Creams and ointments. Such funds activate blood flow and eliminate spasms.
- Steroid hormones. These drugs are injected into the joint cavity. Thanks to this, you can cope with the aggravation of the disease and eliminate severe pain.
- vasodilators. They contribute to the expansion of joint blood vessels and supply the tissues with useful substances.
Folk and alternative tools
In addition to the usual therapy, you can use the following tools:
- Tinctures and decoctions for internal use. Such foundations can be based on lemon, mummy, honey, herbs.
- Ointments from natural ingredients. To prepare them, you can use eucalyptus oil, aloe, and celandine.
- Baths and poultices. Poultices based on cabbage leaves and chicory baths can be used to stop the symptoms of arthrosis.
Physiotherapy
In the phase of remission, physiotherapy is actively used:
- Shock wave therapy - in this case, the body is affected by sound waves, which provide blood flow to the desired area. This improves the regeneration process of the dermis and stimulates metabolic processes.
- Myostimulation - helps to restore the function of muscle tissue, which is weakened due to the forced reduction of motor activity.
- Phonophoresis - under the influence of a special device, a special drug is injected into the affected area in the form of an ointment or cream.
- Ozone therapy - reduces discomfort and activates cartilage development. This effect is achieved due to the ozone-oxygen composition.
Surgical methods
Due to the ineffectiveness of conservative therapy, surgical interventions are prescribed:
- Puncture - pumping excess fluid out of the joint. Thanks to this, it is possible to stop the pain and normalize physical activity.
- Arthroscopic debridement - involves cleaning the inner joint surface from cartilage elements and washing the cavity with a special solution.
- Periarticular osteotomy - artificial fracture of the femur. After that, they are tied together at a different angle, which minimizes the load on the joint.
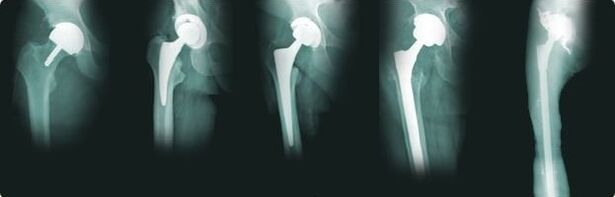
- Endoprosthesis - in this case, the entire joint is replaced with a prosthesis.
Without prosthetic surgery, it is impossible to restore the cartilage tissue in a joint damaged by arthrosis, but with a proper treatment approach, compliance with all medical regulations, appropriate lifestyle, therapeutic exercises, regular massage courses, taking vitamins and proper nutrition, you can stop the process of damage and destruction of the cartilage and hip joints.
Orthopedic products
A cane can be used to relieve stress on the hip joint. In some situations, it is advisable for a person to use crutches.
People with this diagnosis often have to wear a soft bandage. The application of the orthosis helps to reduce the load on the affected area, protects it from dislocations and reduces physical activity.
Effects
In the most difficult situation, a person becomes disabled, completely loses his ability to work and cannot lead an active lifestyle. This condition is very dangerous for the elderly. If you do not help a person, his life expectancy is significantly reduced.
Forecast
The pathology has a favorable prognosis for life. In addition, the disease usually progresses slowly. However, in certain situations, there is a risk of aseptic necrosis of the femur, which is life-threatening.
Arthrosis of the hip joint is a serious pathology that can cause a complete loss of motor activity. To avoid this, you should consult your doctor in time and strictly follow his recommendations.



















